Compare 10 HIPAA-ready, EHR-aware tools for healthcare contact center automation in 2026. See pricing, integrations, ROI, and how to choose.

Healthcare organizations face a perfect storm of rising patient call volumes, persistent staffing shortages, and increasing operational costs. Patients are left waiting on hold, front desk staff are overwhelmed, and revenue is lost to scheduling gaps and claim denials. The traditional call center model is breaking. This is where modern, AI powered healthcare call center solutions come in, transforming patient access and revenue cycle management by automating the repetitive phone work that burdens your team. These platforms aren’t just about answering calls, they are about resolving patient needs and complex payer inquiries efficiently, securely, and at scale.
Healthcare call center solutions are specialized communication platforms designed to manage the unique demands of patient and payer interactions. Unlike generic call center software, these systems are built with healthcare workflows in mind. They go beyond simple phone trees, offering intelligent automation, deep integration with Electronic Health Records (EHRs), and strict adherence to security standards like HIPAA. A modern solution can handle everything from scheduling appointments and verifying insurance benefits to following up on unpaid claims, acting as a digital extension of your administrative team.
When evaluating healthcare call center solutions, look for platforms that address both front office and back office needs. The goal is to find a comprehensive system that streamlines operations across the board.
Healthcare Trained AI Voice Agents: Look for agents pre trained on specific medical workflows, like patient scheduling, benefits verification, or prior authorization follow up. For example, a system with a dedicated agent for scheduling can handle inbound appointment requests 24/7 with zero wait time, reportedly dropping call abandonment rates by as much as 89%.
Deep EHR and PMS Integration: The solution must seamlessly connect with your existing systems. The best platforms offer native integrations with over 80 major EHRs and Practice Management systems, including Epic, athenahealth, Cerner, and NextGen. This ensures patient data is read and written back accurately without manual effort.
Automated Quality Assurance: Top tier solutions include AI powered Quality Assurance that reviews 100% of calls. This ensures every interaction meets accuracy and compliance standards, a massive improvement over the manual spot checking of human agents.
No Code Workflow Customization: Your needs will change. A platform with a no code interface allows your operations team to adjust call scripts and workflows without needing to involve engineers, speeding up deployment and adaptation.
Omnichannel Communication: While voice is critical, the ability to follow up with patients via SMS or email for reminders or confirmations creates a more complete and effective patient engagement strategy.
In healthcare, security is not optional. Any solution that handles Protected Health Information (PHI) must be built on a foundation of robust security and compliance. Your vendor must be willing to sign a Business Associate Agreement (BAA) as required by HIPAA.
Key security features to demand include:
HIPAA and SOC 2 Type II Compliance: This is the gold standard, demonstrating that a vendor has undergone rigorous third party audits of their security controls and processes.
Data Encryption: All data, whether it is at rest in a database or in transit over a network, should be protected with strong encryption protocols like AES 256.
Secure Deployment Options: Look for vendors that offer flexibility, including secure cloud hosting and on premise deployment for health systems with stricter data governance policies.
Zero Day Data Retention Agreements: When using third party AI models, it is critical to ensure your data is not retained or used for training. Vendors like Prosper AI have 0 day data retention agreements with their AI partners to protect your information.
Choosing the right partner is as important as choosing the right technology. During your due diligence process, ask potential vendors tough questions about their experience, support, and security posture.
How many healthcare organizations have you deployed with?
Can you provide case studies or testimonials from clients similar to us?
What does your implementation process look like and who will be my main point of contact?
Describe your security architecture and data breach notification process.
How do you ensure the accuracy of the information your AI agents collect and provide?
A trustworthy partner will have clear, confident answers and will be transparent about their technology and processes.
A standalone healthcare call center solution creates more problems than it solves. True value is unlocked through deep integration. Your chosen platform must function as a natural extension of your core health IT infrastructure.
This means it should have a proven ability to connect to your EHR, Practice Management (PM), and RCM systems. This allows an AI agent to, for example, check a provider’s real time availability in the scheduling system, verify a patient’s eligibility through a clearinghouse connection, and write a structured note back into the patient’s record in the EHR after a call. Without this two way communication, your team is still stuck with manual data entry, defeating the purpose of automation.
The right healthcare call center solutions can make a measurable impact across your organization, from the front desk to the billing office.
AI Appointment Scheduling: Automate inbound and outbound scheduling calls to fill provider calendars, reduce no shows by up to 30%, and handle patient backlogs without hiring more staff.
Patient Re engagement: Proactively call patients who are overdue for preventative care or follow up visits, which can increase booked appointments by over 20%.
24/7 Answering Service: Provide patients with instant, intelligent assistance after hours for scheduling, billing questions, and prescription refill requests.
Benefits Verification: Automate calls to payers to verify eligibility and benefits. Leading AI solutions can complete these calls with 99% accuracy in under two hours, a 50% cost reduction compared to manual work.
Prior Authorization: Automatically initiate and follow up on the status of prior authorizations, reducing the administrative delays that lead to care gaps and claim denials.
Claims and Denial Follow Up: Deploy AI agents to check the status of aging claims and even push back on simple payer errors, helping teams collect up to 15% more on denied claims.
As you narrow down your options, evaluate vendors against a consistent set of criteria to ensure you are making an apples to apples comparison.
Healthcare Exclusivity: Does the vendor focus solely on healthcare? Generic platforms often lack the specific workflow knowledge and compliance features needed.
Time to Value: How quickly can you go live? Some platforms require months of custom development, while others, like Prosper AI, can launch pilot programs in just a few days and full integrations in about three weeks.
Proven ROI: Can the vendor demonstrate measurable results? Look for concrete claims like cost reduction, increased collection rates, or reduced call abandonment. Y Combinator backed Prosper AI, for instance, cites a 50% cost reduction and 3x productivity gain for its clients.
Scalability: Will the solution grow with you? Ensure the platform can handle increasing call volumes and an expanding number of use cases without a degradation in performance.
Support and Management: Do they provide a dedicated manager to help you optimize performance? Having an expert partner is key to maximizing your investment in healthcare call center solutions.
A successful implementation starts with a clear strategy.
Start with a Pilot: Begin with one or two high pain, high volume workflows, such as appointment reminders or benefits verification. This allows you to prove the concept and build momentum.
Define Clear KPIs: Establish baseline metrics before you start. Know your current call abandonment rate, cost per call, and average hold time so you can accurately measure the impact of the new solution.
Involve Your Team: Get buy in from your front desk, call center, and billing teams. Frame the new technology as a tool that frees them from repetitive tasks to focus on higher value patient interactions.
Establish Governance: Designate an owner for the platform internally. Thanks to no code tools, this doesn’t have to be an IT person. An operations leader can often manage and adapt AI agent workflows to meet changing business needs.
The success of your new healthcare call center solution should be measured in both quantitative and qualitative terms. Track key performance indicators (KPIs) to monitor operational efficiency and financial impact.
Operational KPIs:
Call Abandonment Rate
Average Speed to Answer
First Call Resolution Rate
Agent Containment Rate (percentage of calls fully handled by AI)
Financial KPIs:
Cost Per Call/Interaction
Patient Collection Rate
Reduction in Claim Denial Rate
Increase in Scheduled Appointments
Compliance Outcomes:
Maintain a clear audit trail of all automated patient communications.
Use QA scores to ensure adherence to internal scripts and regulatory requirements.
Pricing for advanced healthcare call center solutions is typically usage based and depends on the specific workflows and call volumes you plan to automate. While some organizations may hesitate at the initial investment, the return on investment (ROI) is often rapid and significant.
Consider the “cost of inaction”: the continued expense of staff turnover, the lost revenue from unfilled appointments, and the financial impact of delayed or denied claims. When a single AI agent can do the work of multiple full time employees at a fraction of the cost and with higher accuracy, the financial case becomes clear. Look for platforms that can deliver tangible value within weeks, not years.
To address the growing complexity of patient access and the high turnover in medical front offices, health systems are increasingly turning to specialized automation platforms. The following list features the top ten healthcare call center solutions, grouped for their exceptional ability to handle high call volumes while maintaining strict clinical compliance and EHR connectivity. These industry-leading tools allow practices to streamline their communication workflows, ensuring that every patient inquiry is handled with the precision and speed required in modern healthcare.
Prosper AI brings healthcare‑native voice agents to the front lines of patient access and RCM, taking calls from hold‑music to handled. Beyond simple triage, it completes end‑to‑end tasks: scheduling and referral coordination, insurance and benefits verification, billing Q&A, claims status follow‑ups, and clinical operations like prior auth or pharmacy coordination. This allows staff to focus on care, not call volume.
Connects & compliance
EHR/PM: 80+ native integrations including Epic, athenahealth, eClinicalWorks, Cerner, NextGen, MEDITECH
Telephony & CCaaS: Plugs into existing stacks as a seamless voice layer
Data & APIs: API, FHIR, SFTP for secure, bi‑directional data flows
Security & Hosting: HIPAA with BAA; SOC 2 Type II; end‑to‑end encryption; hybrid deployment with US data residency and audit logs
Outcomes & time‑to‑value
Providers report 50 to 70% automation of inbound calls and 99% accuracy navigating complex payer IVRs. Pilots launch in one to two days via file‑based workflows; full EHR‑integrated rollouts typically complete in three to six weeks.
Pricing & best fit
Usage‑based pricing with custom tiers for high‑volume orgs. Best for health systems, large MSOs, and RCM firms intent on offloading on‑hold labor, accelerating patient access, and reducing burnout.
Hyro’s adaptive conversational AI is engineered for hospital call centers, marrying a linguistic engine with a healthcare knowledge graph to automate what keeps phones ringing. It books and reschedules appointments, powers physician search, manages prescription refills, and handles portal resets, intelligently routing routine requests to SMS to lighten the load on patient access and RCM teams.
Connects & compliance
EHR/PM: Epic (App Market), Oracle Cerner, athenahealth, eClinicalWorks, MEDITECH Expanse
Telephony & CCaaS: Genesys Cloud, Salesforce Health Cloud, Cisco, NICE CXone, Five9, Twilio via SIP/vXML
Data & APIs: Webhooks; FHIR‑based interoperability
Security & Hosting: HIPAA/BAA; SOC 2 Type 2; GDPR/CCPA; PII redaction; SSO; US‑based cloud
Outcomes & time‑to‑value
Health systems report 85% automation, 88% lower abandonment, and 5 to 11x ROI in six months. Pilots typically go live in two to four weeks, with full production under 90 days.
Pricing & best fit
Tiered subscriptions start around $90,000 to $120,000 annually based on skills and channels. Ideal for large health systems and multi‑specialty groups processing 50k+ monthly calls that demand deep clinical interoperability and quick time‑to‑value.
Talkdesk Healthcare Experience Cloud is a purpose‑built CCaaS that synchronizes clinical data with every conversation. It streamlines patient access and RCM with EHR write‑back scheduling, proactive reminders, billing inquiry automation, and benefits verification. Meanwhile, intelligent routing gives agents the full patient context to coordinate complex care journeys with fewer handoffs.
Connects & compliance
EHR/PM: Epic (App Market), Cerner, Salesforce Health Cloud
Telephony & CCaaS: Cloud‑native WebRTC; SIP trunking; BYOC
Data & APIs: FHIR exchange; REST APIs; SFTP; webhooks
Security & Hosting: HIPAA/BAA; HITRUST CSF; SOC 2 Type II; PCI‑DSS; SSO/SAML; AWS cloud/VPC
Outcomes & time‑to‑value
Organizations typically see a 20 to 30% AHT reduction via EHR screen pops. Enterprise deployments land in 60 to 120 days, helped by prebuilt clinical integrations and a cloud‑first architecture.
Pricing & best fit
Per‑seat monthly subscriptions plus telephony usage. Best for mid‑to‑large providers, payers, and high‑volume RCM teams needing secure, deep EHR sync and enterprise‑grade automation.
Nuance, now part of Microsoft, brings medical‑grade conversational AI to the switchboard. Tuned for clinical language and patient intent, it automates appointment scheduling, AI‑driven physician routing, and prescription refills, and it also answers billing questions, processes payments, and powers outreach to close care gaps, easing pressure on patient access and clinical staff.

Connects & compliance
EHR/PM: Epic (App Orchard), Oracle Health (Cerner), MEDITECH
Telephony & CCaaS: Genesys Cloud, Cisco Webex, Avaya, Microsoft Teams (certified connectors)
Data & APIs: HL7, FHIR, SFTP for clinical data exchange
Security & Hosting: HIPAA/BAA; HITRUST CSF; SOC 2 Type II; ISO 27001; SSO/audit logs; Azure cloud‑native
Outcomes & time‑to‑value
Health systems report 30 to 50% IVR containment for routine tasks and 40% fewer abandoned calls. Enterprise pilots typically launch in 12 to 16 weeks, depending on EHR depth.
Pricing & best fit
Custom, tiered pricing by volume and chosen voice/digital modules. Suited for IDNs and AMCs needing deep EHR automation, rigorous security, and scale for massive call volumes.
Orbita’s clinical‑grade conversational AI powers the digital front door, automating pivotal touchpoints before, during, and after care. It books appointments, triages symptoms, guides procedure prep, verifies insurance, and fields billing FAQs, which deflects routine calls from overburdened switchboards while lifting engagement with governed, healthcare‑specific dialogue flows.
Connects & compliance
EHR/PM: Bi‑directional Epic, Cerner, MEDITECH, athenahealth, NextGen via FHIR/HL7
Telephony & CCaaS: Five9, Genesys Cloud CX, Amazon Connect, NICE CXone; SIP/PSTN
Data & APIs: REST APIs, SFTP, webhooks for CRM/marketing ties
Security & Hosting: HIPAA/BAA; SOC 2 Type 2; ISO 27001; SSO (SAML/OAuth); cloud SaaS with VPC options
Outcomes & time‑to‑value
Customers report a 30% cut in admin inefficiencies and response rates rising from 30% to 70%+. Basic modules deploy in days; EHR‑integrated scheduling pilots typically hit production in 8 to 12 weeks.
Pricing & best fit
Tiered subscriptions by interaction volume or functional modules. A fit for large health systems, academic centers, and specialty groups seeking clinical‑grade governance across omnichannel journeys.
Weave acts like a “front office in a box” for busy practices. It reduces no‑shows with smart reminders and confirmations, gives staff instant context via Call Pop, automates recall for follow‑ups, and speeds collections with Text‑to‑Pay, consolidating phones, SMS, and payments to make patient access and RCM run like one connected workflow.
Connects & compliance
EHR/PM: 50+ integrations including athenahealth, Dentrix, DrChrono, AdvancedMD, Eaglesoft; developer REST API
Telephony & CCaaS: Enterprise VoIP with smart routing, recording, AI transcription/sentiment
Data & APIs: REST for custom sync and analytics
Security & Hosting: HIPAA/BAA; SOC 2 Type II; TLS 1.2+/AES‑256; multi‑tenant cloud
Outcomes & time‑to‑value
Practices see a 50% reduction in manual insurance verification time and fewer no‑shows. Typical go‑lives land in two to four weeks, capturing missed‑call revenue quickly.
Pricing & best fit
Tiered plans (Pro, Elite, Ultimate) start around $249/month per location. Best for independent practices and small MSOs in dental, optometry, and specialty medicine consolidating telephony, SMS, and billing.
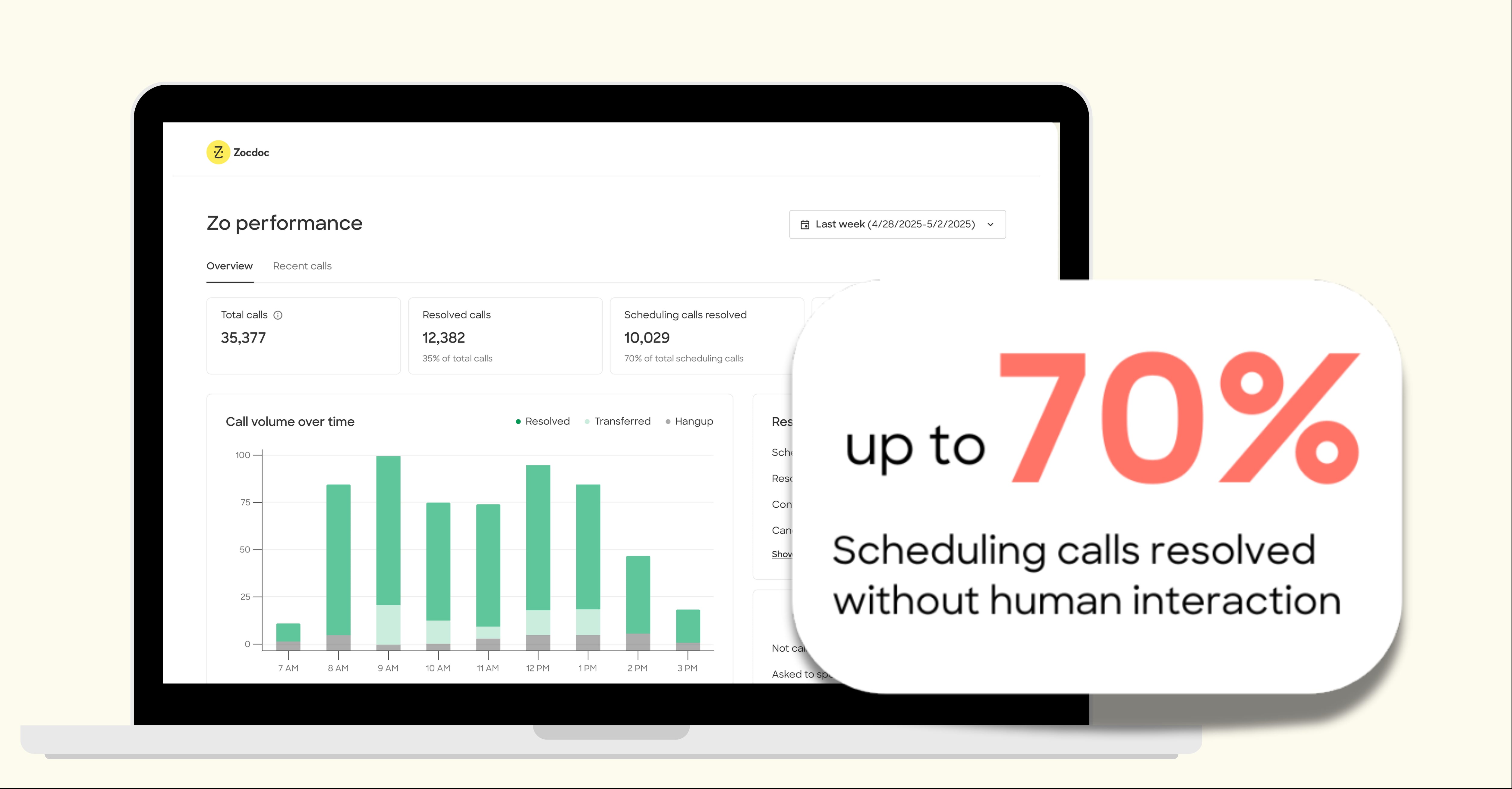
Zo is Zocdoc’s voice‑first AI phone assistant that answers practice lines 24/7 with no hold music required. It books, reschedules, and cancels appointments with Zocdoc’s proven logic, manages intelligent routing and waitlists to fill last‑minute gaps, and is expanding into refills and outbound checkup reminders to curb leakage.
Connects & compliance
EHR/PM: 175+ systems including Epic, athenahealth, Cerner, NextGen
Telephony & CCaaS: Works with any platform via PSTN or SIP
Data & APIs: Enterprise API; FHIR; secure SFTP reporting
Security & Hosting: HIPAA with BAA; SOC 2 Type II; TLS/AES‑256; SSO; audit logs; secure SaaS cloud
Outcomes & time‑to‑value
Zo autonomously resolves up to 70% of scheduling calls (often in under four minutes), cutting abandonment dramatically. Most orgs pilot or go live in two to four weeks with plug‑and‑play integrations.
Pricing & best fit
Outcome‑based at $2 per managed appointment, no upfront fees. Ideal for high‑volume specialty groups, MSOs, and health systems scaling access without adding headcount.
My AI Front Desk is a virtual receptionist for medical and dental practices that never misses a ring. It schedules via booking links, answers FAQs about insurance and hours, triages after‑hours calls, and routes urgent issues to the right nurse line. This gives lean teams a dependable first layer that lifts both patient experience and staff capacity.
Connects & compliance
EHR/PM: Jane, Zocdoc, Calendly, custom portals; Zapier to 5,000+ CRM/EHR apps
Telephony & CCaaS: Works with any landline/VoIP via call forwarding; dedicated local numbers
Data & APIs: Zapier automations; transcript/SMS logging
Security & Hosting: HIPAA with BAA; encrypted transcripts; secure cloud console access
Outcomes & time‑to‑value
Practices report 100% answer rates and a 40 to 60% reduction in front‑desk workload. Go‑live can take under 30 minutes, often just by uploading existing FAQs.
Pricing & best fit
Flat $54.99/month. Perfect for solo practitioners, small clinics, and dental offices seeking enterprise‑grade call automation without CCaaS complexity or cost.
Amelia turns healthcare contact centers into always‑on, AI‑assisted hubs. Using advanced NLP, it handles end‑to‑end scheduling, prescription refills, and intake, while offloading RCM tasks like eligibility checks, billing inquiries, and proactive reminders, so patients get answers fast and staff reclaim hours.
Connects & compliance
EHR/PM: Bi‑directional Epic, Oracle Health (Cerner), athenahealth via FHIR APIs
Telephony & CCaaS: Genesys, Five9, Avaya, Cisco; SIP/PSTN
Data & APIs: FHIR, REST, SFTP for secure batch transfers
Security & Hosting: HIPAA/BAA; HITRUST CSF; SOC 2 Type II; SSO; audit logs; cloud/VPC options
Outcomes & time‑to‑value
Typical results: 70 to 85% containment on routine inquiries and up to 30% fewer no‑shows and abandoned calls. Prebuilt modules support pilots that reach production in 6 to 10 weeks.
Pricing & best fit
Usage‑based (per interaction/minute) or tiered subscriptions. A strong match for large health systems, MSOs, and payer contact centers needing a human‑like voice interface for complex access and RCM workflows.
Druid AI delivers verticalized voice and chat agents built specifically for healthcare’s front lines. The platform connects patient conversations with back‑end clinical systems to automate scheduling, billing inquiries, real‑time eligibility checks, and AI‑driven switchboard routing, which reduces repetitive work while preserving governed, compliant workflows.
Connects & compliance
EHR/PM: Epic (App Market), Oracle Health (Cerner), MEDITECH via FHIR/HL7
Telephony & CCaaS: Genesys Cloud CX, Five9, Avaya
Data & APIs: FHIR, SFTP; extensible integrations; SSO audit logs
Security & Hosting: HIPAA/BAA; SOC 2 Type II; ISO 27001; deploy to multi‑tenant cloud (Azure/AWS), VPC, or on‑prem
Outcomes & time‑to‑value
Health systems often reach 60 to 80% containment for routine requests and cut no‑shows by 20 to 30%. Prebuilt healthcare templates speed design‑to‑pilot windows to four to eight weeks.
Pricing & best fit
Tiered subscriptions priced by interaction volume or “active digital workers.” Ideal for mid‑to‑large providers and healthcare BPOs requiring strict data residency and complex EHR interoperability.
The world of healthcare call center solutions is evolving quickly. Looking ahead, we can expect to see even more sophisticated capabilities become mainstream. This includes more proactive and predictive outreach, where AI can identify patients at risk of missing appointments or non compliance and engage them preemptively. We will also see tighter integrations with clinical data, allowing for more personalized and context aware conversations. As the technology matures, these AI powered solutions will become an indispensable part of the healthcare administrative infrastructure.
Navigating the complexities of patient communication and payer relations requires more than just a good phone system. It requires intelligent, secure, and integrated healthcare call center solutions designed for the unique challenges of the industry. By automating repetitive phone based workflows, you can empower your staff to work at the top of their license, improve patient satisfaction, and strengthen your organization’s financial health. Choosing the right platform is a critical step in building a more efficient and resilient healthcare operation.
Ready to see how AI voice agents can transform your patient access and RCM workflows? Explore the platform at Prosper AI.
A healthcare call center solution is a specialized software platform designed to manage patient and payer phone communications. Unlike generic systems, it includes features for HIPAA compliance, EHR integration, and automation of specific healthcare workflows like appointment scheduling, benefits verification, and claims follow up.
AI can dramatically improve a healthcare call center by automating high volume, repetitive calls. This leads to 24/7 availability for patients, zero hold times, reduced staff burnout, lower operational costs, and higher accuracy on data collection tasks.
Yes, reputable healthcare call center solutions are designed to be HIPAA compliant. Look for vendors that will sign a Business Associate Agreement (BAA) and have certifications like SOC 2 Type II to verify their security practices.
Implementation times vary. While complex, custom builds can take months, some modern AI platforms can launch initial pilot programs in as little as a few days and achieve full integration with an EHR in about three weeks.
Absolutely. Integration with your EHR and Practice Management system is a critical feature. Leading solutions offer dozens of pre built, native integrations with major systems like Epic, Cerner, athenahealth, and NextGen, enabling seamless data flow.
The key differences are specialization and compliance. Healthcare call center solutions are pre trained on medical terminology and workflows, understand the complexities of dealing with payers, and have the necessary security architecture like HIPAA and SOC 2 compliance built in from the ground up.
Discover how healthcare teams are transforming patient access with Prosper.

Compare 10 HIPAA-ready, EHR-aware tools for healthcare contact center automation in 2026. See pricing, integrations, ROI, and how to choose.

Discover 10 best AI scheduling for clinics tools in 2026—HIPAA-ready, EHR-integrated, voice-first options with ROI and pricing. Compare picks to choose yours.

Compare 10 AI Insurance Verification tools for 2026—voice agents and portal/API engines. See pricing, HIPAA/SOC 2, EHR integrations, and best fits. Read now.