
As we move through 2026, artificial intelligence is no longer an experiment in healthcare; it’s a core component of modern delivery systems. A dedicated healthcare AI platform can automate burdensome administrative tasks, enhance patient access, and streamline revenue cycle management, allowing providers to focus on what matters most: patient care. With the digital health market expected to exceed $300 billion in 2026, driven largely by AI, health systems are strategically deploying solutions to combat workforce shortages and financial pressures. This guide will walk you through the essential components of a healthcare AI platform, how to evaluate them, and which use cases deliver the most significant impact.
At its core, a healthcare AI platform must ensure the confidentiality, integrity, and availability of Protected Health Information (PHI). HIPAA compliance isn’t an optional feature; it’s a foundational requirement for any technology handling sensitive patient data. The regulations don’t have specific rules for AI, but the existing Privacy, Security, and Breach Notification Rules apply just as they would to any other system.
Business Associate Agreement (BAA): Any third party vendor providing a healthcare AI platform that handles PHI must sign a BAA. This is a legal contract certifying they will safeguard PHI according to HIPAA standards.
Data Encryption: PHI must be encrypted both “at rest” (when stored) and “in transit” (when being transmitted). This prevents unauthorized access even if the underlying infrastructure is compromised.
Access Controls: Platforms must enforce strict access controls, ensuring users can only view the “minimum necessary” amount of PHI required for their jobs. This includes features like role based access and two factor authentication.
Audit Trails: The system must log all access to PHI, creating a transparent record of who accessed what data and when. These audit trails are crucial for security monitoring and breach investigations.
Choosing a platform without these safeguards isn’t just a security risk; it’s a direct violation of federal law that can lead to severe penalties.
Beyond basic HIPAA rules, a robust healthcare AI platform must adhere to a higher standard of security and governance. This means looking for vendors that can demonstrate a mature approach to risk management.
Essential Certifications and Practices:
SOC 2 Type II: This certification validates that a vendor has effective security controls in place over time.
GDPR Compliance: For organizations that serve patients in Europe, compliance with the General Data Protection Regulation is non negotiable.
Data Retention Policies: A vendor should have clear policies on data retention, including how long data is stored and how it is securely destroyed. For instance, a zero day retention agreement with underlying AI model providers like OpenAI ensures sensitive data isn’t held longer than necessary.
Regular Security Audits: The platform should undergo regular penetration testing and vulnerability scans to proactively identify and fix security weaknesses.
Strong governance ensures the AI is not only compliant but also safe, ethical, and aligned with your organization’s commitment to patient care.
One of the most significant risks in 2026 is the rise of “shadow AI”. This refers to the use of AI tools by staff outside of the organization’s official oversight. Employees trying to be more efficient might use consumer grade AI tools like public chatbots to summarize notes or draft patient communications.
This practice is incredibly dangerous. Using unapproved tools for work involving PHI can lead to:
Data Breaches: Consumer AI tools lack the necessary security safeguards, making them prime targets for data breaches.
HIPAA Violations: Uploading PHI to a public AI tool without a BAA is a clear HIPAA violation.
Inaccurate Outputs: Generic AI models are not trained on validated medical information and can produce biased or clinically incorrect information, threatening patient safety.
Organizations must establish clear policies and provide approved, enterprise grade tools to prevent staff from turning to risky alternatives. A dedicated healthcare AI platform like Prosper AI gives your team the efficiency they need within a secure, compliant environment.
Choosing the right healthcare AI platform requires a structured evaluation. Don’t get distracted by hype; focus on the fundamentals that ensure a successful partnership.
Healthcare Experience: Does the vendor understand the complexities of the healthcare environment, including clinical workflows and regulatory demands?
Clinical and Technical Validation: Is the AI clinically validated, and can the vendor explain how their models work? Look for transparency and a track record in live clinical settings.
Integration Capabilities: How easily does the platform integrate with your existing infrastructure, particularly your EHR? A vendor should have proven experience with major systems like Epic, Cerner, and athenahealth.
Scalability and Support: Can the platform support your organization as it grows? What level of support and training does the vendor provide during and after implementation?
Transparent Pricing: The vendor should offer a clear cost model without hidden fees. While usage based pricing is common, you should be able to get accurate cost estimates.
A healthcare AI platform is only as effective as its ability to connect with your core systems. Seamless EHR integration is the most critical piece. Without it, the AI cannot access the data it needs to function or write structured results back into the patient record.
When evaluating a platform, ask about:
EHR and PM System Experience: Look for a vendor with a deep library of existing integrations.
Interoperability Standards: The platform should support modern standards like HL7 FHIR to ensure data can be exchanged reliably.
Implementation Process: A good partner will have a clear, structured process for integration, with dedicated project managers and technical specialists to work with your IT team.
A platform designed for interoperability avoids creating yet another data silo, instead unifying your technology stack and making workflows more efficient.
A successful rollout goes beyond technology. It requires a thoughtful approach to change management and governance. Successful AI innovators dedicate 70% of their effort to people and processes, not just algorithms.
Involve End Users Early: Get feedback from the clinicians, front desk staff, and billing teams who will use the platform daily. Their insights are invaluable for ensuring the tool is practical and addresses real world challenges.
Start with a Pilot: Begin with a focused pilot project in a specific department to prove value and work out any kinks before a full scale deployment.
Establish a Governance Committee: Create a formal oversight group with representatives from clinical, IT, compliance, and operations to manage the AI strategy.
Provide Thorough Training: Ensure all users are trained not only on how to use the platform but also on the policies governing its use.
To justify the investment in a healthcare AI platform, you need to track the right Key Performance Indicators (KPIs). Success isn’t just about financial return; it also encompasses operational efficiency and patient outcomes.
Call Abandonment Rate: For patient access use cases, a primary goal is to ensure every patient gets a response. AI agents can reduce abandonment rates by answering calls instantly.
Patient No Show Rate: Missed appointments cost the U.S. healthcare system over $150 billion annually. AI powered reminders and scheduling can reduce no shows significantly.
Cost Per Claim/Authorization: For revenue cycle tasks, measure the reduction in cost to verify benefits, submit a prior authorization, or check a claim’s status.
Denial Rate: Track the percentage of claims denied due to administrative errors like missing prior authorizations or incorrect eligibility information.
Patient Collections: Measure the increase in patient balance collections and the reduction in accounts receivable days.
Platforms like Prosper AI provide dashboards and analytics to track these metrics in near real time, demonstrating clear ROI (see case studies for proof points).
The most effective way to deploy a healthcare AI platform is to target specific, high‑volume workflows where administrative burden is highest (see common healthcare AI use cases to prioritize your roadmap).
AI Appointment Scheduling: AI voice agents can handle inbound and outbound scheduling calls 24/7, reducing wait times and filling provider calendars. Some health systems have seen an 89% drop in call abandonment after implementing AI schedulers.
Appointment Reminders: Automated, interactive reminders via voice, SMS, or email can cut no‑show rates by up to 30%.
Patient Re engagement: Proactively contact patients who are overdue for care to fill schedule gaps and improve population health outcomes.
Benefits & Eligibility Verification: Automate phone calls to payers to verify patient benefits, capturing dozens of data points with near‑perfect accuracy and cutting costs by over 50%.
Prior Authorization Automation: AI agents can navigate payer IVRs and speak with representatives to initiate and follow up on prior authorizations, reducing care delays. Some AI tools have demonstrated a 45% faster clinical analysis for these requests.
Claims Status and Denial Follow up: AI can automatically check the status of aging claims and even push back on payers for improper denials, increasing collections.
The Total Cost of Ownership (TCO) for a healthcare AI platform extends beyond the initial subscription or licensing fee. When budgeting, consider the full lifecycle costs.
Initial Fees: This includes software licenses, implementation costs, and any required hardware upgrades.
Integration Costs: Factor in the staff time and resources from your IT department needed to connect the platform to your EHR and other systems.
Training and Change Management: Account for the time required to train your staff and adapt workflows.
Ongoing Maintenance and Support: This includes annual subscription fees and any costs for system updates or support from the vendor.
While some organizations may hesitate at the upfront investment, a comprehensive TCO analysis often reveals a compelling return. By reducing manual labor, increasing collections, and improving provider capacity, the right healthcare AI platform can deliver a significant ROI.
As we transition from theoretical applications to real-world impact, identifying the standout tools becomes essential for operational excellence. This curated selection highlights the top five platforms leading the charge in 2026 by integrating seamless automation with clinical precision. These solutions are grouped here because they represent the most robust and scalable capabilities for modernizing healthcare workflows today.
Prosper AI brings voice‑first automation to U.S. healthcare, putting AI phone agents to work across Patient Access and RCM. Through voice and IVR, agents schedule visits, verify benefits, pursue prior authorizations, and follow up on claims, navigating payer menus and speaking with live reps when needed. Prosper AI lists more than 80 native connections and can unlock bidirectional updates with EHR or PM APIs. enable structured write‑backs that keep downstream workflows in sync.
Where it shines
Automates scheduling, reminders, and outreach with 0-second wait time for appointment scheduling and direct EHR write‑backs.
Traverses payer IVRs for eligibility, PA status, and denial follow-up with reported 99% accuracy.
Connects natively to Epic, Cerner, athenahealth, MEDITECH via FHIR/HL7/SFTP for reliable data exchange.
AI‑driven QA on every call with near‑real‑time dashboards, transcripts, and operational insights.
Enterprise security & compliance
HIPAA with BAA; SOC 2 Type II; encryption in transit and at rest; SSO/RBAC.
Zero‑retention options with model providers; daily backups; identity provider integration.
Deploy in secure cloud or on‑prem to meet enterprise and residency requirements.
Verify: PHI retention/redaction settings, residency constraints, and audit‑log granularity.
What results to expect
Customers report up to 50% cost reductions and 89% lower abandonment. Typical go‑live lands in ~3 weeks with prebuilt EHR/PM connections. Best fit: health systems and large specialty groups modernizing access/RCM by phone. Pricing is volume‑based and quote‑driven.
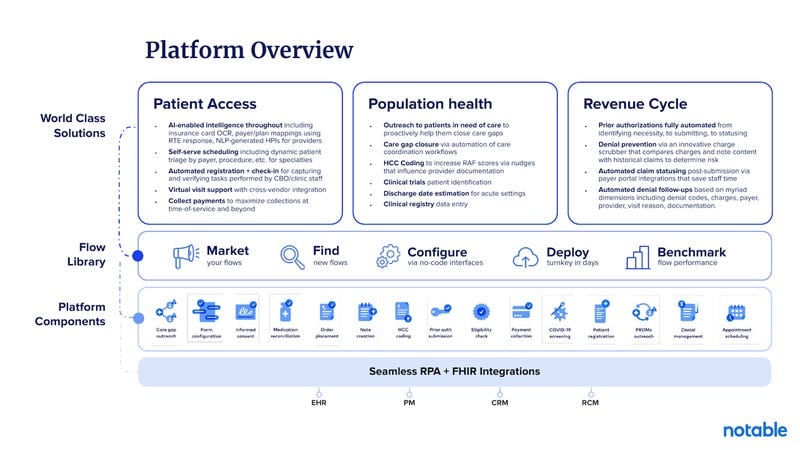
Notable is an enterprise automation platform for providers, orchestrating patient access, revenue cycle, and care ops in one fabric. Patient Access and RCM leaders deploy voice and SMS flows to handle intake, scheduling, eligibility, and authorizations, without swivel‑chair data entry. Deep, bi‑directional EHR integrations keep work in‑workflow for Epic‑heavy organizations.
Where it shines
End‑to‑end RCM automation: digital intake, referral triage, 270/271 eligibility, and 278 prior authorizations.
Omnichannel Contact Center AI: inbound/outbound voice agents and SMS for appointments and billing Q&A.
Deep connectivity with Epic, Cerner, athena; supports FHIR, HL7, X12, and OCR for document handling.
Low‑code Flow Builder + Connector Hub with 786+ healthcare-specific integrations and REST APIs for scale.
Enterprise security & compliance
HIPAA with BAAs; SOC 2 Type II, ISO 27001, HITRUST; encryption; RBAC and SSO.
Multi‑region U.S. hosting for availability and residency; independent testing and pentests.
Governance via versioning, controlled rollouts, and real‑time Insights monitoring.
Verify: PHI retention/redaction settings, residency constraints, and audit‑log granularity.
What results to expect
Organizations see 57% call containment and 35%+ touchless authorizations. Typical go‑lives in 2 to 6 weeks. Best for IDNs/AMCs and large systems with Epic footprints seeking measurable RCM lift. Pricing is quote‑based for providers.
Waystar’s Auth Accelerate equips Patient Access and RCM teams with end‑to‑end medical prior authorization automation. It programmatically determines requirements, submits requests, and returns statuses, embedded directly in Epic and MEDITECH. Staff manage PAs inside familiar EHR workflows while a rules engine handles payer variability at scale.
Where it shines
Full‑cycle automation: requirement checks, initiation, and 30 service lines covered.
AltitudeAI rules engine with 6M+ rules for payer variability and medical necessity checks.
Seamless Epic/MEDITECH connectivity using X12, including automated clinical attachments.
600+ payer portals accessed to accelerate submissions and cut manual work.
Enterprise security & compliance
HITRUST CSF and SOC 2 Type II; regular third‑party audits and penetration testing.
HIPAA with BAAs; encryption in transit/at rest; enterprise SSO and RBAC.
Verify: PHI retention/redaction settings, residency constraints, and audit‑log granularity.
What results to expect
Customers cite 70% faster submissions and 85% auto‑approvals, driving fewer denials and faster TAT. Strong fit for Epic/MEDITECH health systems seeking measurable PA lift. Pricing is quote‑based per module.
Surescripts Touchless Prior Authorization automates pharmacy‑benefit medication PAs directly within e‑prescribing workflows. By extracting relevant clinical data and transmitting it to PBMs and health plans, it eliminates phone/fax back‑and‑forth for prescribers and access teams. A web portal supports practices lacking native EHR features.
Where it shines
Automates medication PAs by matching EHR data to payer criteria; median approval time of 18 seconds.
Embedded ePA in certified e‑prescribing keeps clinicians in-workflow, with no switching to fax or phone.
Deep Epic, Cerner, athenahealth integration using NCPDP SCRIPT for nationwide interoperability.
Leverages Real‑Time Prescription Benefit and Specialty Medications Gateway to streamline complex therapies.
Enterprise security & compliance
HIPAA/BAA; HITRUST r2 and SOC 2 Type II; encryption at rest and in transit.
Standards‑first: NCPDP SCRIPT across the Surescripts Network Alliance and major EHRs.
EHNAC and DirectTrust accreditations; encrypted troubleshooting logs for data integrity.
Verify: PHI retention/redaction settings, U.S. residency, and SSO/RBAC granularity in admin portals.
What results to expect
Approval cycles drop from days to seconds, cutting physician abandonment and denials. Ideal for large systems and high‑volume specialties managing complex meds. Deployment is rapid via existing EHR connectivity. Pricing is quote‑based.
Cohere Health is a payer‑side clinical intelligence platform that modernizes prior authorization and utilization management. Health plans and provider networks plug in via web portals and EHR‑embedded experiences (e.g., Epic Payer Platform). FHIR‑based APIs accelerate evidence‑based decisions while preserving auditability and regulatory alignment.
Where it shines
Intelligent decisioning automates 50–90% of approvals, reducing manual reviews and appeals.
EHR integration through Epic Payer Platform and SMART on FHIR keeps clinicians in‑workflow.
CMS‑aligned, FHIR‑first APIs support CMS‑0057‑F and Da Vinci/HL7 implementation guides.
Clinical rigor at scale using MCG guidelines across MSK, cardiology, and radiology, serving 600k+ providers.
Enterprise security & compliance
HITRUST r2; NCQA/URAC accreditations for UM and platform security.
AES‑256 at rest, TLS 1.2+ in transit; enterprise SSO and role‑based access controls.
Built for CMS Interoperability rules with HL7 FHIR‑based, standardized data exchange.
Verify: PHI retention/redaction settings, residency requirements, and field‑level audit‑log detail.
What results to expect
Plans report up to 90% automation and 47% administrative cost reductions. Best for regional/national payers modernizing UM and meeting CMS timelines. Deployments accelerate via Epic connectivity and FHIR rails. Pricing is quote‑based, typically per covered life.
The healthcare AI platform landscape is evolving rapidly. Looking ahead, two major trends will define the next generation of technology: generative AI and agentic AI.
Generative AI: While early applications focused on automating documentation, GenAI is becoming a “copilot” for clinicians and administrators. It can synthesize clinical notes, streamline communications, and surface care gaps.
Agentic AI: This represents a shift from single task AI tools to autonomous systems that can manage complex workflows. An AI agent could orchestrate the entire prior authorization process, from identifying the need for an auth to submitting the request and scheduling the approved procedure, with minimal human intervention.
As these technologies mature, they will become more deeply embedded in care delivery, making the selection of a secure, enterprise grade healthcare AI platform more critical than ever.
In 2026, a specialized healthcare AI platform is no longer a luxury but a necessity for health systems looking to thrive amidst financial pressures and staffing shortages. By automating repetitive phone based workflows in patient access and revenue cycle management, these platforms free up staff, reduce administrative waste, and create a better experience for patients. When choosing a solution, prioritize vendors with deep healthcare expertise, a proven security posture, and seamless EHR integration. A platform built on these principles will not only solve today’s challenges but also provide a foundation for adopting the next wave of AI innovation.
Ready to see how a purpose‑built healthcare AI platform can transform your operations? Explore the AI voice agents from Prosper AI or Get started today.
A healthcare AI platform is a specialized software solution that uses artificial intelligence to automate administrative and clinical workflows. These platforms are designed to be HIPAA compliant and integrate with existing systems like EHRs to handle tasks such as appointment scheduling, benefits verification, and claims management.
HIPAA (Health Insurance Portability and Accountability Act) is a federal law that sets the standard for protecting sensitive patient data. An AI platform that handles PHI must have technical, physical, and administrative safeguards in place to ensure data is kept private and secure, including encryption and strict access controls. Failure to comply can result in massive fines and reputational damage.
The primary benefits include significant cost reduction, improved operational efficiency, and an enhanced patient experience. AI can automate tasks that cost the U.S. healthcare system hundreds of billions in administrative waste annually. This frees up staff from time consuming phone calls, reduces patient hold times, and ensures tasks like prior authorizations are completed quickly and accurately.
Integration is typically achieved through secure connections like APIs or HL7 interfaces. This allows the AI platform to read necessary patient and schedule information from the EHR and write structured data, such as appointment confirmations or benefits details, back into the patient’s record. Deep integration is key to a seamless workflow.
A general AI chatbot is not built to handle sensitive health information and lacks the security, compliance, and workflow specific training required for healthcare. A true healthcare AI platform is HIPAA compliant, signs a BAA, and features AI agents pre trained on specific medical workflows, like navigating complex insurance payer phone systems.
By automating high volume, repetitive tasks, a healthcare AI platform acts as a force multiplier for your existing staff. AI voice agents can handle hundreds of simultaneous calls for scheduling, billing questions, or status checks, allowing your front desk and back office teams to focus on more complex patient interactions and operate at the top of their license.
Look for a vendor with a proven track record in healthcare, robust security certifications like SOC 2 Type II, and a deep library of successful EHR integrations. They should be transparent about their AI models, provide excellent support, and offer a clear pricing structure.
Implementation times can vary. Solutions that use batch data uploads can go live in a matter of days. A full integration with an EHR via API typically takes a few weeks to configure and test thoroughly. A good vendor will provide a clear timeline and a dedicated manager to guide the process.
Discover how healthcare teams are transforming patient access with Prosper.

Compare the top AI Agent Healthcare tools for 2026—workflows, HIPAA, pricing, and real results for patient access and RCM. Find your fit.

Compare healthcare contact center solutions in 2026: AI voice agents, CCaaS, messaging, and triage. See picks, pricing signals, and how to choose.